Americans are once again facing huge bills for COVID-19 treatment as insurers that previously volunteered to waive out-of-pocket costs rapidly opt out.
Early in the pandemic, the vast majority of people in fully insured private plans would have had their treatment completely covered, the nonprofit Kaiser Family Foundation found.
Today, 94% of the insurers it examined are billing again — and another 2% will start billing by March.
With the omicron variant sweeping the country, here’s how you can keep your costs low if you end up needing care.
Why are insurers charging again?
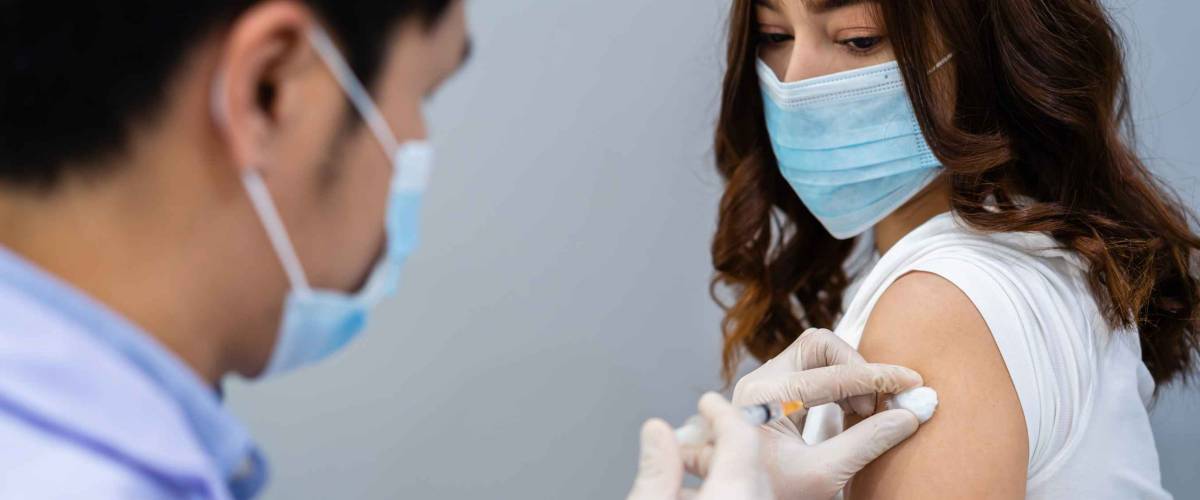
To help stop the spread, the U.S. government ensures COVID-19 vaccines are completely free of charge. The same goes for COVID-19 testing.
This, however, is not true for treatment. While a handful of states demanded insurers waive cost sharing for patients, most of the companies that did so nationwide acted voluntarily.
Insurers may have feared heavy-handed government intervention if they didn’t act first by volunteering, the Kaiser Family Foundation suggests.
Now, with vaccines widely available, insurers may no longer feel as much pressure to pay for illnesses that could have been avoided or reduced in severity by getting jabbed.
Must Read
- Dave Ramsey warns nearly 50% of Americans are making 1 big Social Security mistake — are you doing the same?
- Thanks to Jeff Bezos, you can now become a landlord for as little as $100 — and no, you don't have to deal with tenants or fix freezers. Here's how
- Robert Kiyosaki says this 1 asset will surge 400% in a year and begs investors not to miss this ‘explosion’
Join 250,000+ readers and get Moneywise’s best stories and exclusive interviews first — clear insights curated and delivered weekly. Subscribe now.
How much does COVID-19 care cost?
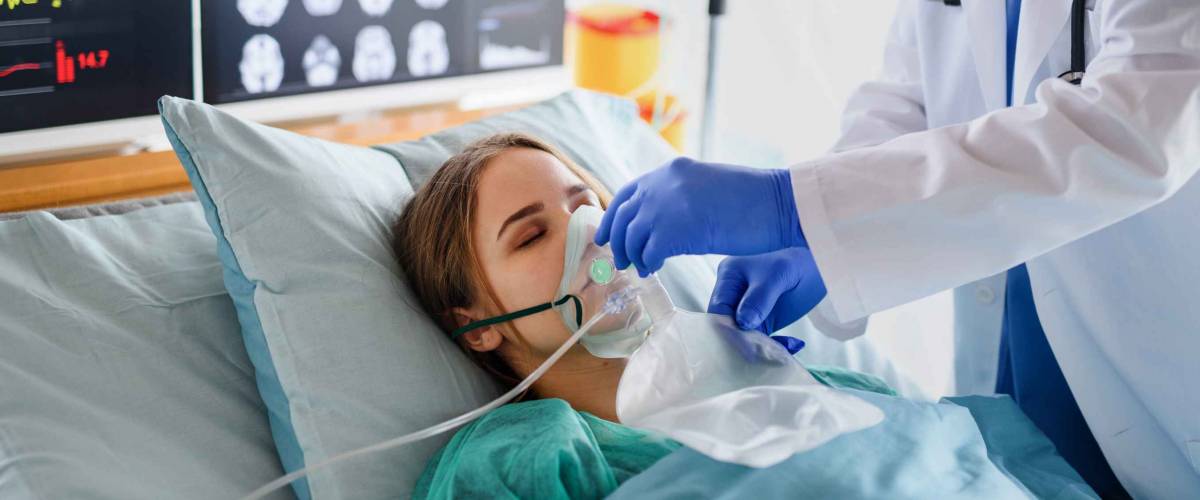
With waivers quickly coming to an end, patients will need to pay any fees associated with their standard health insurance policy. That means your deductible, coinsurance and copayments plus the cost of any services that aren't covered.
How much can that be? It depends on how severe your illness is. While the highly infectious omicron variant is considered less potent, the delta variant has yet to disappear completely.
Early in the pandemic, a woman named Janet Mendez told The New York Times that she spent 19 nights in hospital and needed to use a ventilator. Her medical bills totaled over $400,000, but with insurance she expected to pay under $10,000.
Casey Gray told CNN in May that he was hospitalized for 75 days, racking up a whopping $3,400,000 bill. He too ended up paying about $10,000, due to his insurance.
A study last year found those without cost-sharing waivers paid an average of $3,800 out of pocket if they had private insurance and an average of $1,500 if they had a Medicare Advantage plan.
For those with a marketplace plan, the maximum you can be asked to pay this year is $8,700 for an individual and $17,400 for a family. Some plans have even lower limits.
How to protect yourself

While most out-of-pocket waivers are long gone, there’s plenty you can do to ensure you won’t suffer a mammoth bill on top of getting sick.
If you don’t have insurance, get it
Out-of-pocket costs can be painful, but the damage will be much, much worse if you don’t have coverage at all.
For a patient without insurance, the average cost of a COVID-19 hospital stay early in the pandemic was about $73,300, a FairHealth study found.
While open enrollment for marketplace plans has ended, you may still be able to lock in affordable health insurance if you've recently lost health coverage, moved, got married or had a baby.
If you absolutely can’t secure insurance at the moment, you can try asking your medical provider to bill the government’s HRSA COVID-19 Uninsured Program.
However, only certain providers are participating, not all of your medical costs may be covered, and it won't protect you from other illnesses and injuries.
If you do have insurance, rethink your coverage
Now that insurers aren’t waiving out-of-pocket costs, you’ll likely need to cover a few thousand dollars in deductibles, copays and coinsurance.
If you have a high-deductible plan, consider upgrading to get a lower deductible. Or you may want to consider switching to a plan without a copay.
These choices do come with a higher premium — but thanks to government relief efforts, marketplace plans are even more affordable than usual.
Premiums are currently limited to no more than 8.5% of your income, and millions more people can take advantage of generous subsidies.
Again, while open enrollment has ended, you can still switch to a new or better marketplace plan if you qualify for a special enrollment period.
It’s worth a few minutes to compare plans and providers to see how much further your money can go — a strategy that could also save you as much as $1,000 a year on your car insurance and home insurance.
You May Also Like
- Turning 50 with $0 saved for retirement? Most people don’t realize they’re actually just entering their prime earning decade. Here are 6 ways to catch up fast
- Inside a $1B real estate fund offering access to thousands of income-producing rental properties — with flexible minimums starting at $10
- Vanguard’s outlook on U.S. stocks is raising alarm bells for retirees. Here’s why and how to protect yourself
- Here are 5 easy ways to own multiple properties like Bezos and Beyoncé. You can start with $10 (and no, you don’t have to manage a single thing)
Chris Murray was formerly a freelance contributor with Moneywise.

Investing • Dec 29
Best short-term investment strategies for 2024

Investing • Jun 13











